Normal Heart Rate and Respiratory Rate in Dogs: AI-COLLAR Study Results
Our paper Resting heart and respiratory rates in dogs in their natural environment: new insights from a long-term, international, prospective study in a cohort of 1012 dogs using a biometric device for longitudinal non-invasive cardiorespiratory monitoring (AI-COLLAR), published in Frontiers in Veterinary Science (2025), Frontiers, establishes the first global baseline for normal heart rate and respiratory rate values in apparently healthy dogs. Conducted with Professor Valerie Chetboul, it is powered by the Invoxia Biotracker GPS for Dogs, winner of the CES Innovation Award 2024.
We monitored 703 healthy dogs across Europe, North America, and Asia - including 42% in France and 29% in the United States - day and night for up to a year thanks to the Invoxia Biotracker. The result is an unprecedented real-world dataset: normal cardiac rate and breathing rate reference values tracked by age, weight, sex, breed, circadian rhythm, and even season for dogs living in the Northern Hemisphere, plus distinct profiles uncovered in 129 cardiac dogs.
Just like connected devices are transforming human medicine, this study shows how predictive veterinary care becomes possible: individualized monitoring, early alerts, and scalable real-world data to protect every dog. Thank you to the dedicated dog parents whose commitment made AI-COLLAR possible.

Inside the AI-COLLAR study in numbers
The AI-COLLAR cohort delivers an unmatched scientific baseline for normal heart rate and respiratory rate values in dogs:
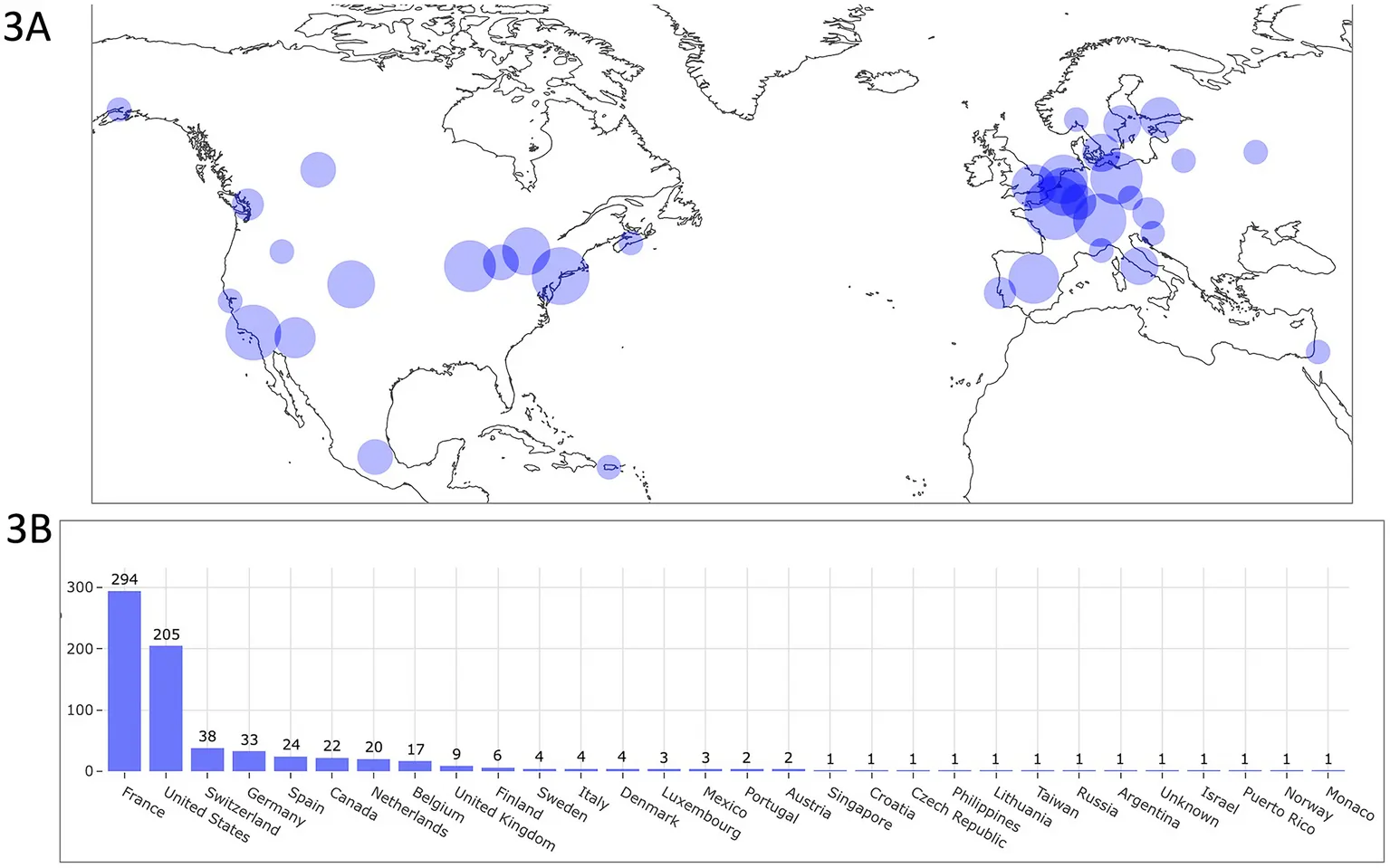
- 703 healthy dogs monitored in their natural environment.
- 29 countries, including 42% in France and 29% in the United States.
- 189 days median wear time per dog, spanning 113 breeds and every life stage.
Collected far from clinic stress, these data points define the physiological references that preventive veterinary medicine was missing.
What is a normal heart rate in dogs? What is a normal respiratory rate?
These are the questions every dog parent and veterinarian asks. The AI-COLLAR study provides the first comprehensive answers, establishing normal resting heart rate (RHR) and respiratory rate (RRR) values for dogs in their everyday lives.
| Characteristics | Sub-groups | Number of dogs | Heart rate (bpm) | Respiratory rate (Brpm) |
|---|---|---|---|---|
| Sex | Male dogs | 314 | 60.3 [54.7–65.2] | 16.0 [13.7–18.4] |
| Female dogs | 248 | 60.7 [56.2–65.4] | 16.1 [14.0–18.7] | |
| Time of measurement | Nighttime | 533 | 58.3 [53.6–64.2] | 14.2 [12.1–17.0] |
| Day time | 533 | 61.3 [56.3–66.7] | 17.4 [15.2–19.8] | |
| Dog size category | Large-sized dogs (> 20 kg) | 355 | 59.5 [54.7–63.8] | 15.6 [13.7–18.4] |
| Small- to medium-sized dogs (≤20 kg) | 207 | 62.1 [56.4–68.1] | 16.5 [14.5–19.0] | |
| Medium to large-sized dogs (>10 kg) | 478 | 59.5 [54.6–64.2] | 15.8 [13.7–18.3] | |
| Small-sized dogs (≤10 kg) | 84 | 65.0 [60.9–69.4] | 17.2 [15.0–19.9] | |
| Health status | Apparently healthy dogs | 562 | 60.5 [55.2–65.3] | 16.1 [13.8–18.7] |
| Diseased dogs | 166 | 65.4 [60.0–78.5] | 17.5 [14.6–20.9] | |
| Apparently healthy dogs | 562 | 60.5 [55.2–65.3] | 16.1 [13.8–18.7] | |
| Dogs with heart diseases | 129 | 67.3 [61.0–81.5] | 18.0 [14.9–21.5] |
How age reshapes vital signs
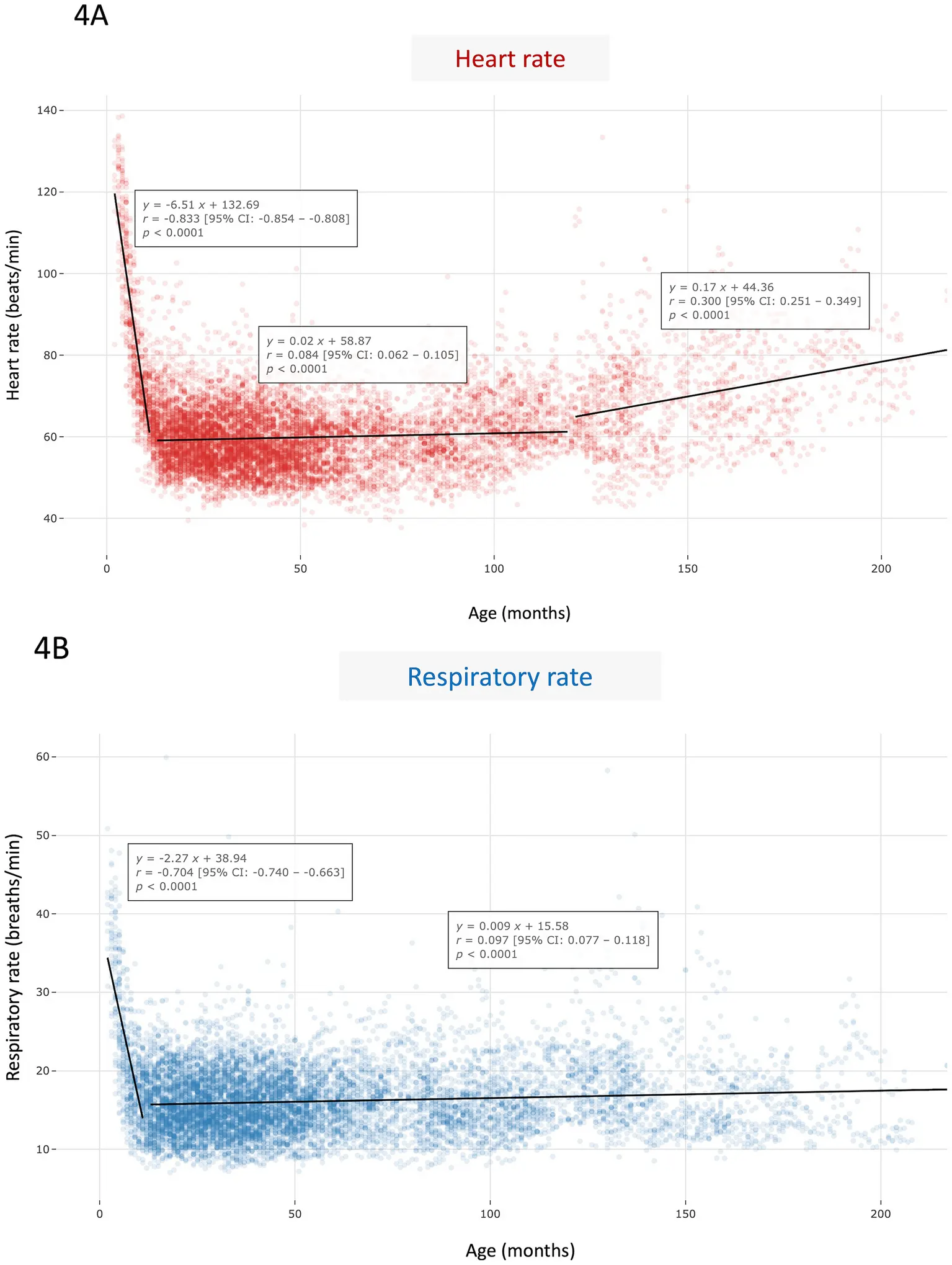
Longitudinal tracking highlights distinct profiles in both heart rate and breathing:
- Puppies (≤ 12 months) drop sharply, with median heart rate falling from 78.5 to 59.1 beats per minute. Respiratory rate also decreases in parallel, from about 22.6 to 15.3 breaths per minute, showing how young dogs quickly settle into calmer physiology.
- Adults (1–10 years) stabilize, with heart rate holding around 60 beats per minute and respiratory rate near 16 breaths per minute.
- Seniors (≥ 10 years) show a gentle rise, with heart rate climbing up to 68.7 beats per minute and respiratory rate also trending upward, reaching 17.4 breaths per minute.
Tracking how both constants evolve with age allows deviations to be flagged long before they escalate.
Understanding these age-specific normal heart rate ranges lets you flag deviations long before they escalate.
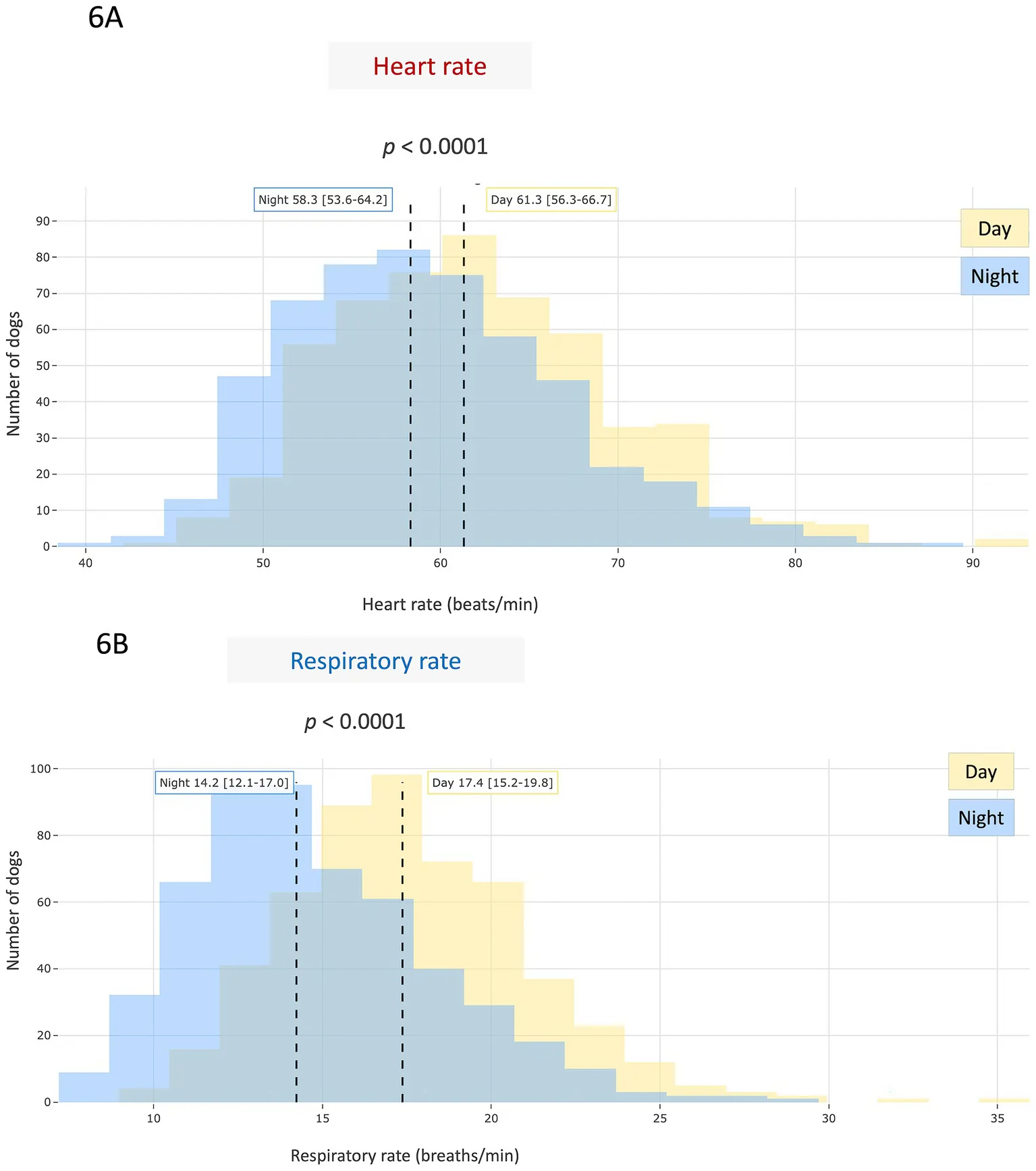
Day vs Night: Understanding the circadian pattern
Continuous monitoring reveals a clear signal: both heart rate and breathing rate fall significantly at night. This circadian signature reflects deep rest and balanced autonomic tone.
Normal heart and respiration rates are lower during nighttime sleep compared to daytime resting.
Every Heartbeat Matters
Invoxia Biotracker continuously monitors your dog’s cardiac health - detecting irregular rhythms, tracking respiratory rates, and alerting you to changes that could save their life. Peace of mind, clipped to their collar.

Healthy Heart Rate and Respiratory Rate by Weight and Breed: Weight and breed leave their mark
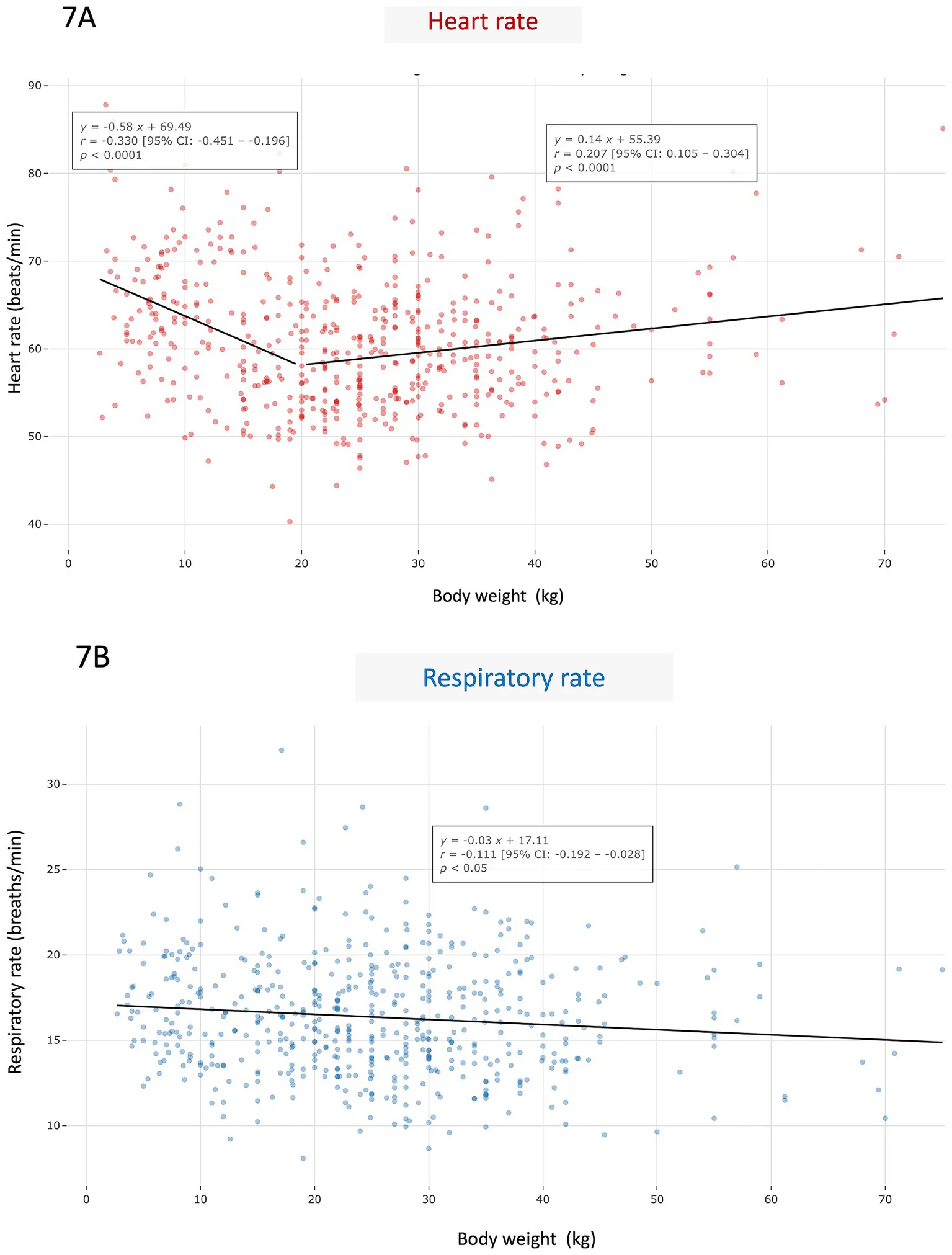
Weight class and genetics shape normal heart rate and breathing rate baselines:
- Large dogs (> 20 kg) display lower cardiac rate and respiratory rate values than smaller companions.
- Golden Retrievers, Australian Shepherds and Border Collies show the lowest normal resting heart rates.
- Australian Shepherds have higher normal breathing rates, while Dobermans breathe slower.
Interpreting an individual dog’s rates range requires a reference built on similar weight and breed profiles, which is exactly what the AI-COLLAR dataset provides.
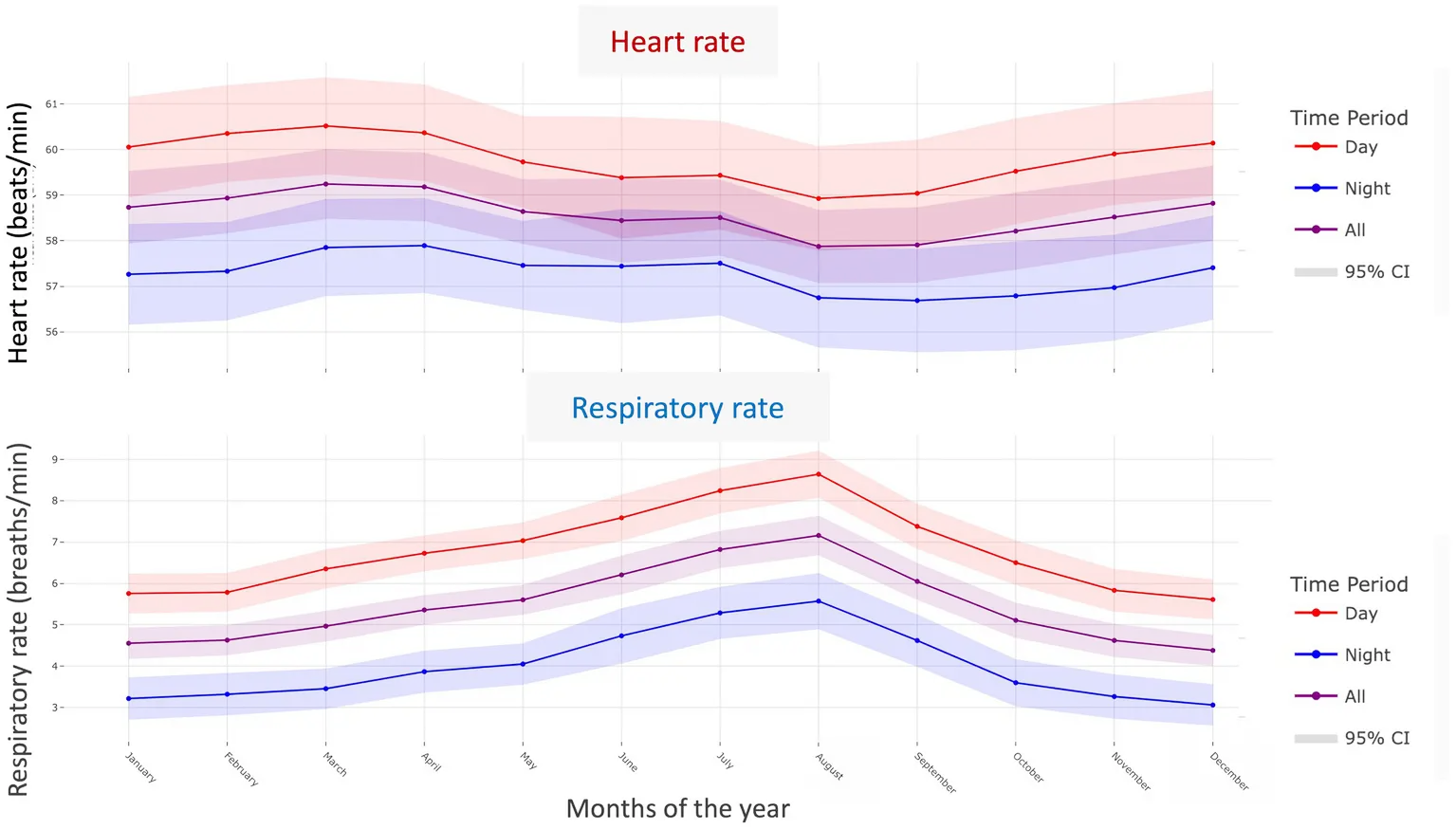
Seasonal Variations in Normal Rates: Seasons influence every heartbeat
In the Northern Hemisphere the heart rate dips across summer while the respiratory rate climbs from April and peaks in August. Thermal panting is a healthy response to hotter days.
Knowing these seasonal normal cardiac rate and breathing rate patterns prevents false alarms and speeds up intervention when something truly deviates from normal ranges. Our algorithms contextualize each measurement with climate effects.
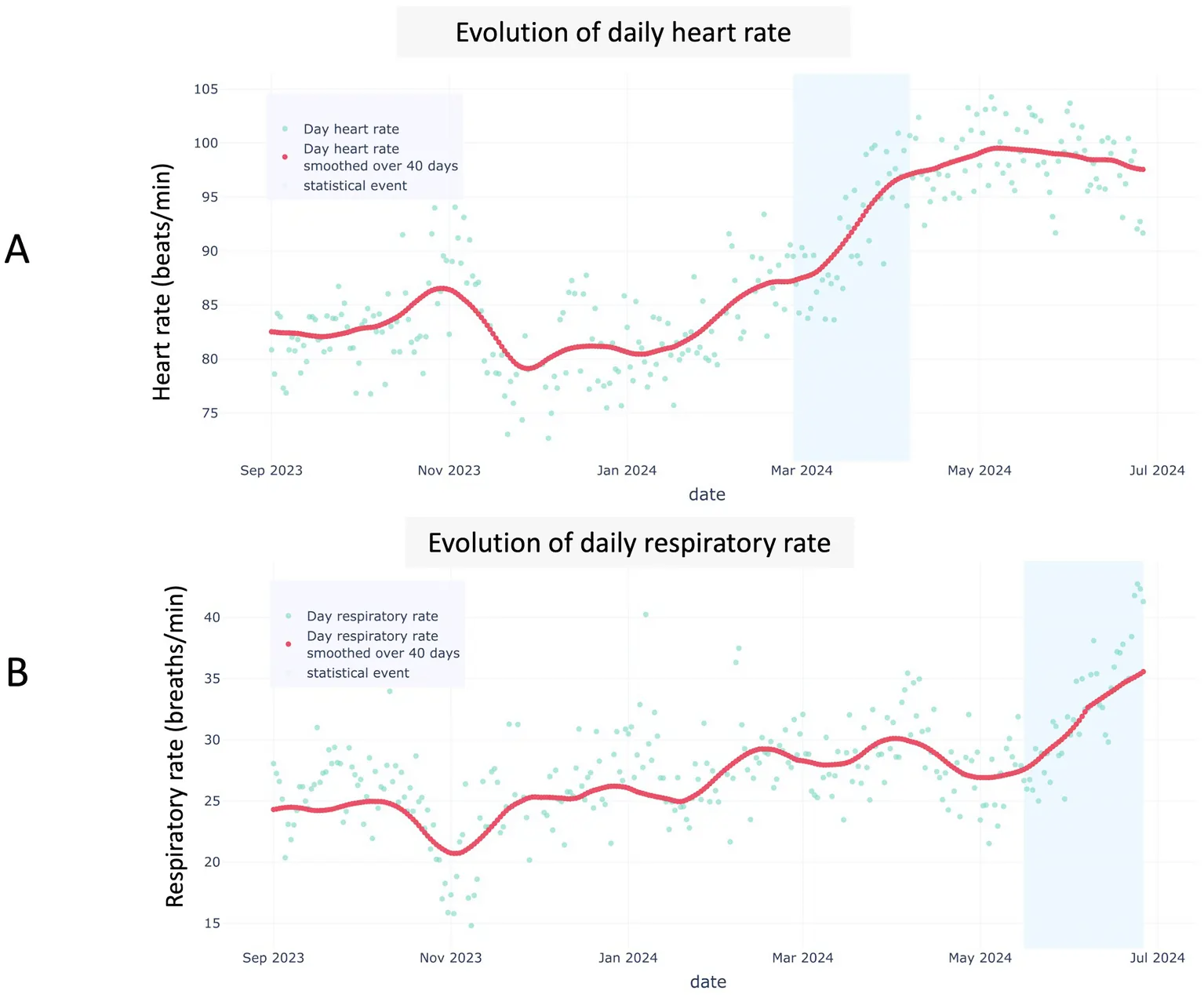
AI-powered early detection
Dogs with cardiac conditions exhibit elevated resting heart rate (RHR) and Respiration Rate (RRR) long before visible symptoms. The Invoxia Biotracker catches those weak signals early.
- 120 days before pulmonary edema, the algorithm spotted a continuous resting HR rise.
- 129 dogs living with heart disease helped build personalized thresholds.
The result? Alerts delivered before the clinical emergency, giving veterinarians precious time to act.
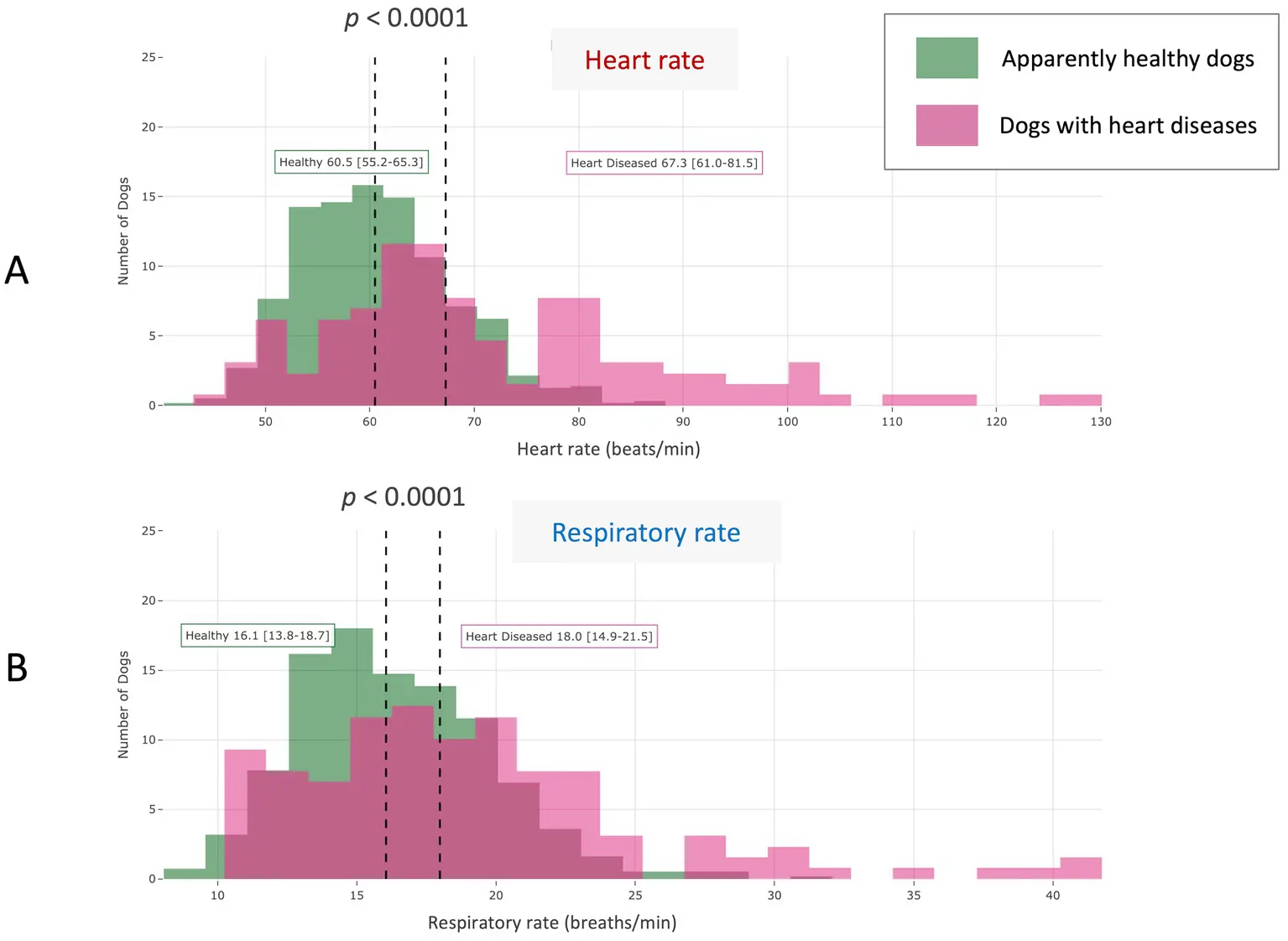
When Rates Deviate from Normal: Enabling preventive, predictive veterinary care
We also compared healthy dogs with those diagnosed with heart conditions, and the findings show clear deviations from normal heart rate values:
- Dogs with heart disease had resting heart rates above normal ranges for their age and weight.
- Their respiratory rates were elevated compared to normal values in healthy dogs.
These shifts in vital signs are closely linked to disease and may appear even before visible symptoms. This suggests that continuous monitoring of heart rate and breathing rate averages could help spot problems earlier, enabling veterinarians and dog parents to take action before the condition worsens.
How the Invoxia Biotracker GPS for Dogs keeps your dog thriving
The Invoxia Biotracker GPS for Dogs is a non-invasive biometric monitor. Our sensor leverages seismocardiography to capture micro vibrations on your dog’s neck and convert them into reliable cardio-respiratory metrics.
- Automatic readings whenever your dog is lying calmly.
- AI models trained on the largest canine cohort, delivering 99.6% accuracy for HR and 98.6% for RR.
- Zero friction: clip the collar and get 24/7 health intelligence.
Your dog keeps its routine; you gain medical-grade visibility in real time.
Dive deeper with the scientific paper
Explore the full methodology and results in Frontiers in Veterinary Science: Resting heart and respiratory rates in dogs in their natural environment: new insights from a long-term, international, prospective study in a cohort of 703 dogs using a biometric device for longitudinal non-invasive cardiorespiratory monitoring.
Open-access publishing validates the Invoxia approach and shares this unique knowledge base with the wider veterinary community.
Key reference
- Chetboul V, Humbert E, Dougoud L, Lorre G (2025) Resting heart and respiratory rates in dogs in their natural environment: new insights from a long-term, international, prospective study in a cohort of 703 dogs using a biometric device for longitudinal non-invasive cardiorespiratory monitoring. Frontiers in Veterinary Science, 12:1667355. doi: 10.3389/fvets.2025.1667355. Licensed under CC BY 4.0.
Full bibliography
- Mfouth Kemajou, P, Mbanya, A, and Coppieters, Y. Digital approaches in post-COVID healthcare: a systematic review of technological innovations in disease management. Biol Methods Protoc. (2024) 9:bpae070. doi: 10.1093/biomethods/bpae070
- Lee, NK, and Kim, JS. Status and trends of the digital healthcare industry. Healthc Inform Res. (2024) 30:172-83. doi: 10.4258/hir.2024.30.3.172
- Jensen, MT, Treskes, RW, Caiani, EG, et al. ESC working group on e-cardiology position paper: use of commercially available wearable technology for heart rate and activity tracking in primary and secondary cardiovascular prevention. Eur Heart J Digit Health. (2021) 2:49-59. doi: 10.1093/ehjdh/ztab011
- Schuuring, MJ, Treskes, RW, Castiello, T, et al. Digital solutions to optimize guideline-directed medical therapy prescription rates in patients with heart failure. Eur Heart J Digit Health. (2024) 5:670-82. doi: 10.1093/ehjdh/ztae064
- Bayoumy, K, Gaber, M, Elshafeey, A, et al. Smart wearable devices in cardiovascular care: where we are and how to move forward. Nat Rev Cardiol. (2021) 18:581-99. doi: 10.1038/s41569-021-00522-7
- Hughes, A, Shandhi, MMH, Master, H, Dunn, J, and Brittain, E. Wearable devices in cardiovascular medicine. Circ Res. (2023) 132:652-70. doi: 10.1161/CIRCRESAHA
- Russell, M, Cain, E, Bazzano, L, et al. Collecting at-home biometric measures for longitudinal research from the i3C: feasibility and acceptability study. JMIR Hum Factors. (2025) 12:e71103. doi: 10.2196/71103
- Bhaltadak, V, Ghewade, B, and Yelne, S. A comprehensive review on advancements in wearable technologies: revolutionizing cardiovascular medicine. Cureus. (2024) 16:e61312. doi: 10.7759/cureus.61312
- Scholte, NTB, van Ravensberg, AE, Shakoor, A, et al. A scoping review on advancements in noninvasive wearable technology for heart failure management. NPJ Digit Med. (2024) 7:279. doi: 10.1038/s41746-024-01268-5
- Ortmeyer, HK, Robey, L, and McDonald, T. Combining Actigraph link and PetPace collar data to measure activity, proximity, and physiological responses in freely moving dogs in a natural environment. Animals (Basel). (2018) 8:230. doi: 10.3390/ani8120230
- Rowlison de Ortiz, A, Belda, B, Hash, J, et al. Initial exploration of the discriminatory ability of the PetPace collar to detect differences in activity and physiological variables between healthy and osteoarthritic dogs. Front Pain Res (Lausanne). (2022) 3:949877. doi: 10.3389/fpain.2022.949877
- Belda, B, Enomoto, M, Case, BC, and Lascelles, BDX. Initial evaluation of PetPace activity monitor. Vet J. (2018) 237:63-8. doi: 10.1016/j.tvjl.2018.05.011
- Gunasekaran, T, and Sanders, RA. Assessment of heart rate measurements obtained from a smart collar compared to 24-h Holter monitoring in healthy dogs. J Vet Cardiol. (2025) 57:58-64. doi: 10.1016/j.jvc.2024.11.002
- Jarkoff, H, Lorre, G, and Humbert, E. Assessing the accuracy of a smart 2 collar for dogs: predictive performance for heart and breathing rates on a large scale dataset. Cold Spring Harbor Laboratory. (2023). doi: 10.1101/2023.06.09.544347
- Keene, BW, Atkins, CE, Bonagura, JD, et al. ACVIM consensus guidelines for the diagnosis and treatment of myxomatous mitral valve disease in dogs. J Vet Intern Med. (2019) 33:1127-40. doi: 10.1111/jvim.15488
- Wess, G. Screening for dilated cardiomyopathy in dogs. J Vet Cardiol. (2022) 40:51-68. doi: 10.1016/j.jvc.2021.09.004
- Schober, KE, Hart, TM, Stern, JA, et al. Effects of treatment on respiratory rate, serum natriuretic peptide concentration, and doppler echocardiographic indices of left ventricular filling pressure in dogs with congestive heart failure. J Am Vet Med Assoc. (2011) 239:468-79. doi: 10.2460/javma.239.4.468
- Porciello, F, Rishniw, M, Ljungvall, I, et al. Sleeping and resting respiratory rates in dogs and cats with medically-controlled left-sided congestive heart failure. Vet J. (2016) 207:164-8. doi: 10.1016/j.tvjl.2015.08.017
- Boswood, A, Gordon, SG, Haggstrom, J, et al. Temporal changes in clinical and radiographic variables in dogs with preclinical myxomatous mitral valve disease: the EPIC study. J Vet Intern Med. (2020) 34:1108-18. doi: 10.1111/jvim.15753
- Reynolds, CA, Brown, DC, Rush, JE, et al. Prediction of first onset of congestive heart failure in dogs with degenerative mitral valve disease: the PREDICT cohort study. J Vet Cardiol. (2012) 14:193-202. doi: 10.1016/j.jvc.2012.01.008
- Hezzell, MJ, Humm, K, Dennis, SG, Agee, L, and Boswood, A. Relationships between heart rate and age, bodyweight and breed in 10,849 dogs. J Small Anim Pract. (2013) 54:318-24. doi: 10.1111/jsap.12079
- Ferasin, L, Ferasin, H, and Little, CJ. Lack of correlation between canine heart rate and body size in veterinary clinical practice. J Small Anim Pract. (2010) 51:412-8. doi: 10.1111/j.1748-5827.2010.00954.x
- Lee, PM, and Brown, RHT. Establishing 24-hour Holter reference intervals for clinically healthy puppies. Res Vet Sci. (2019) 125:253-5. doi: 10.1016/j.rvsc.2019.07.010
- Bodey, AR, and Michell, AR. Epidemiological study of blood pressure in domestic dogs. J Small Anim Pract. (1996) 37:116-25. doi: 10.1111/j.1748-5827.1996.tb02358.x
- Montoya Navarrete, AL, Quezada Tristan, T, Lozano Santillan, S, et al. Effect of age, sex, and body size on the blood biochemistry and physiological constants of dogs. BMC Vet Res. (2021) 17:265. doi: 10.1186/s12917-021-02976-w
- Geis, WP, Tatooles, CJ, Priola, DV, and Friedman, WF. Factors influencing neurohumoral control of the heart in the newborn dog. Am J Phys. (1975) 228:1685-9. doi: 10.1152/ajplegacy.1975.228.6.1685
- Hajduczok, G, Chapleau, MW, and Abboud, FM. Rapid adaptation of central pathways explains the suppressed baroreflex with aging. Neurobiol Aging. (1991) 12:601-4. doi: 10.1016/0197-4580(91)90092-x
- Monahan, KD. Effect of aging on baroreflex function in humans. Am J Physiol Regul Integr Comp Physiol. (2007) 293:R3-R12. doi: 10.1152/ajpregu.00031.2007
- Randall, OS, Esler, MD, Bulloch, EG, et al. Relationship of age and blood pressure to baroreflex sensitivity and arterial compliance in man. Clin Sci Mol Med Suppl. (1976) 51:357s-60s. doi: 10.1042/cs051357s
- Rishniw, M, Ljungvall, I, Porciello, F, Haggstrom, J, and Ohad, DG. Sleeping respiratory rates in apparently healthy adult dogs. Res Vet Sci. (2012) 93:965-9. doi: 10.1016/j.rvsc.2011.12.014
- Saikia, D, and Mahanta, B. Cardiovascular and respiratory physiology in children. Indian J Anaesth. (2019) 63:690-7. doi: 10.4103/ija.IJA_490_19
- Noujaim, SF, Lucca, E, Munoz, V, et al. From mouse to whale: a universal scaling relation for the PR interval of the electrocardiogram of mammals. Circulation. (2004) 110:2802-8. doi: 10.1161/01.CIR.0000146785.15995.67
- Goldbogen, JA, Cade, DE, Calambokidis, J, et al. Extreme bradycardia and tachycardia in the world’s largest animal. Proc Natl Acad Sci USA. (2019) 116:25329-32. doi: 10.1073/pnas.1914273116
- Lamb, AP, Meurs, KM, and Hamlin, RL. Correlation of heart rate to body weight in apparently normal dogs. J Vet Cardiol. (2010) 12:107-10. doi: 10.1016/j.jvc.2010.04.001
- Hasegawa, M, Sasaki, M, Umemoto, Y, et al. Exploring sleep heart rate variability: linear, nonlinear, and circadian rhythm perspectives. Front Vet Sci. (2024) 11:1386425. doi: 10.3389/fvets.2024.1386425
- Varga, B, Gergely, A, Galambos, A, and Kis, A. Heart rate and heart rate variability during sleep in family dogs (Canis familiaris). Animals (Basel). (2018) 8:107. doi: 10.3390/ani8070107
- Noszczyk-Nowak, A, Pasawska, U, and Nicpon, J. ECG parameters in 24-hour holter monitoring in healthy dogs. Bull Vet Inst Pulawy. (2009) 53:499-502.
- Ohad, DG, Rishniw, M, Ljungvall, I, Porciello, F, and Haggstrom, J. Sleeping and resting respiratory rates in dogs with subclinical heart disease. J Am Vet Med Assoc. (2013) 243:839-43. doi: 10.2460/javma.243.6.839
- Goldberg, MB, Langman, VA, and Taylor, CR. Panting in dogs: paths of air flow in response to heat and exercise. Respir Physiol. (1981) 43:327-38. doi: 10.1016/0034-5687(81)90113-4
- Parsons, S, Scott, AR, and Macdonald, IA. The effect of posture and environmental temperature on cardiovascular reflexes in normal subjects and diabetes mellitus. Clin Auton Res. (1992) 2:147-51. doi: 10.1007/BF01818954
- Mavropoulou, A, Oliveira, P, and Willis, R. Holter monitoring in dogs: 24 h vs. 48 h. Vet J. (2021) 272:105628. doi: 10.1016/j.tvjl.2021.105628
- Calvert, CA. Heart rate variability. Vet Clin North Am Small Anim Pract. (1998) 28:1409-27. doi: 10.1016/s0195-5616(98)50129-5
- Petrie, JP. Practical application of holter monitoring in dogs and cats. Clin Tech Small Anim Pract. (2005) 20:173-81. doi: 10.1053/j.ctsap.2005.05.006
- Gunasekaran, T, and Sanders, RA. Determining the optimal Holter monitoring duration for detecting ventricular arrhythmia in dogs: a Bayesian approach. J Vet Cardiol. (2025) 60:14-22. doi: 10.1016/j.jvc.2025.05.003